
Topics: Virgin Island, Channel 4, TV And Film, Health, Women's Health, Real Life

Topics: Virgin Island, Channel 4, TV And Film, Health, Women's Health, Real Life
Virgin Island is officially back on our screens - and one contestant has bravely lifted the lid on her experience with vaginismus, which she says has left her 'living life in fear'.
The Channel 4 show follows 12 people who have never had sex as they embark on a unique intimacy course at a luxury Mediterranean retreat.
They take part in a series of intimacy workshops and are teamed up with sexperts, who discuss and work on any fears or barriers they might have.
On Monday (27 April), the second season officially kicked off with a brand new batch of contestants, including 22-year-old event coordinator Joy, who detailed her struggles with the health condition.
Advert
She emotionally explained: "With sexual intimacy, I feel a little bit broken. I can't have sex. I have a condition called vaginismus. If somebody tried to touch my vagina, it would be pain, and it would be discomfort, and I'm living life in fear.
"The way that you're seen as a woman who can't physically have sex is like, what's the point?"

Later, during a session with one of the experts, she elaborated, saying: "I know I have a sexual side to me. I have vaginismus. Vaginismus is a condition related to the pelvic floor and also has a psychological fear component around the idea of insertion or entry.
"The moment that I realised I had vaginismus, it was like this whole idea of a sector of my life that could be, just closed up."
She revealed: "I can't wear a tampon, I can't do a pap smear, and I definitely can't have sex. It's so hard.
"At one point, I literally thought God cursed me with vaginismus. I thought he did it to me to stop me from having sex. It's hard to undo that feeling."
Tyla spoke with an intimate health and women's wellness issues expert, Dr Shirin Lakhani, who explained the details of the little-known condition.
She explained that vaginismus is a condition where the muscles of the pelvic floor involuntarily tighten in response to attempted vaginal penetration.

"This isn’t something a woman is consciously controlling," the expert outlined. "It’s a reflex, often rooted in a complex interplay between physical sensitivity, past experiences, and psychological factors such as anxiety or fear.
"Clinically, it can present as difficulty or inability to insert a tampon, undergo a pelvic examination, or have penetrative sex. For some women, it’s lifelong (primary vaginismus), while for others it develops later (secondary), sometimes triggered by pain, trauma, childbirth, menopause-related changes, or medical conditions affecting the vulva and vagina."
Vaginismus can be caused by a range of both 'physical and psychological factors'.
For example, if you have experienced past trauma, sometimes sexual or medical trauma, this can cause vaginismus, and cultural or religious messaging that can cause fear or anxiety around sex can also have an impact.
"Underlying medical issues could also be the cause, such as hormone dysfunction or Lichen Sclerosus. Getting to the underlying issues can really help to understand and treat vaginismus correctly," the doctor added.
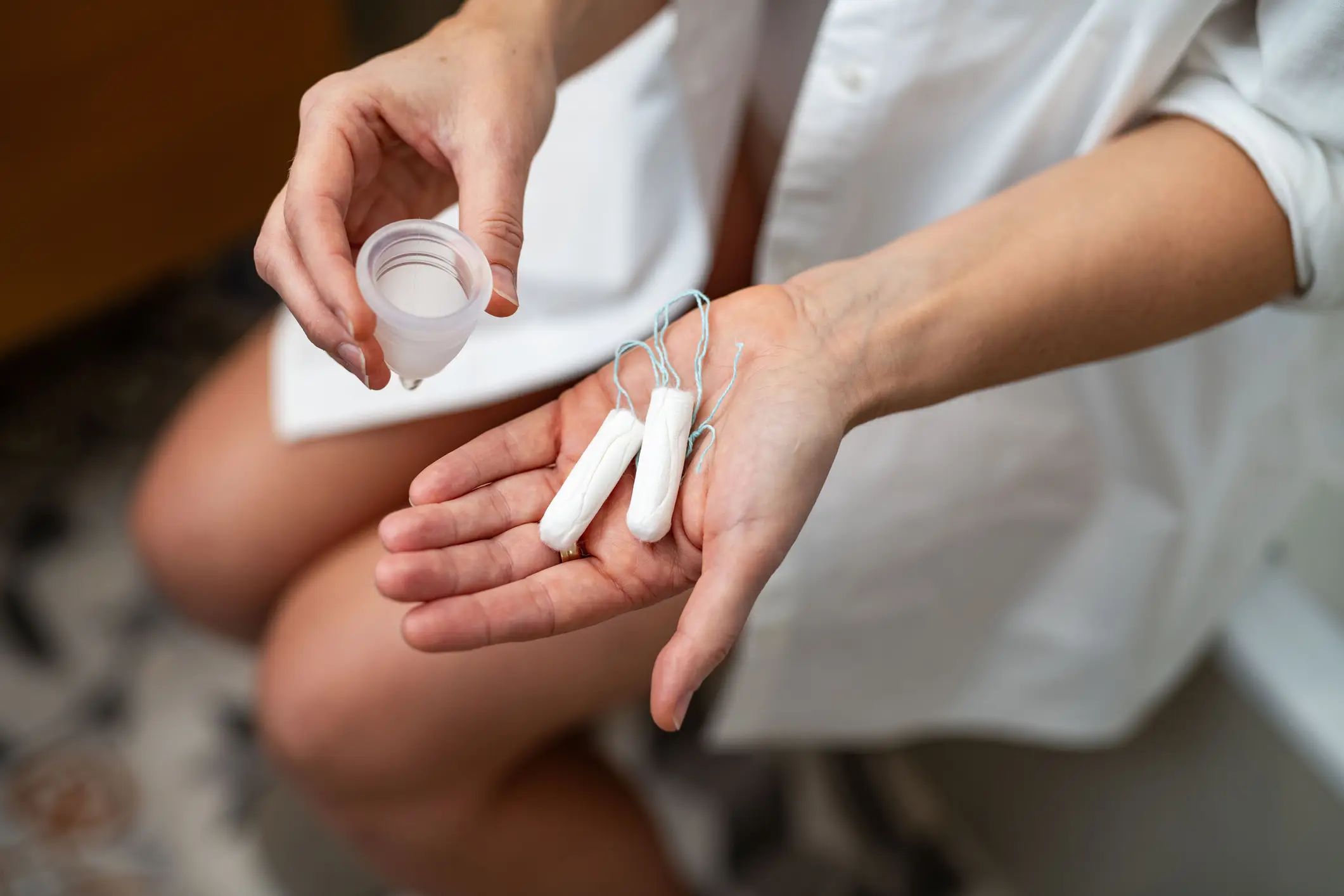
Dr Lakhani explained that vaginismus can make penetrative sex 'difficult, painful, or in some cases impossible'.
She explained: "The key issue is the involuntary tightening of the pelvic floor muscles. This creates a physical barrier to penetration, but it also feeds into a cycle of anticipation, anxiety, and further muscle spasm.
"Vaginismus can affect intimacy, relationships, and self-esteem. Some women begin to avoid sex altogether out of fear of pain, while others feel guilt or frustration, particularly if the condition is misunderstood by partners or dismissed as purely psychological."
Vaginismus is treatable, mainly with pelvic floor exercises and psychosexual therapy.
Dr Lakhani outlined how pelvic floor physiotherapy focuses on 'helping women regain control over the pelvic floor muscles, learning how to consciously relax them, rather than contract'.
She added: "Alongside this, vaginal dilator therapy is often used. These are graduated devices that allow for slow, controlled introduction of penetration in a way that feels safe and manageable.
"There’s also an important psychological component. Psychosexual therapy can help address fear, anxiety, or past experiences that may be contributing to the reflex muscle tightening. Even in cases where there’s a clear physical trigger, the anticipation of pain can perpetuate the cycle."

Doctors can also identify if there are any underlying drivers, such as hormonal changes and conditions like vulvodynia, lichen sclerosus, or recurrent infections.
The expert urges anyone who thinks they might have vaginismus to see their GP.
Dr Lakhani concluded: "Vaginismus is significantly under-discussed and under-represented within healthcare, despite being relatively common.
"Many people go years without diagnosis because many women feel embarrassed about discussing it or seeking help from a medical professional. Women shouldn’t suffer in silence, and I really recommend that if you think you may be suffering from vaginismus, to seek medical advice."