Weight loss drugs have quickly moved from being medical treatments to help manage Type 2 diabetes to one of the most talked-about developments in modern healthcare.
Medications such as Ozempic and Wegovy belong to a class known as GLP-1 receptor agonists, and were originally designed to help people regulate blood sugar.
By working similarly a naturally occurring hormone that controls insulin release, the drugs work by slowing digestion, and signalling fullness to the brain, these drugs were initially prescribed to improve metabolic health, not as a mainstream weight-loss solution.
However we have witnessed a huge change in how these medications are prescribed and used, as clinicians began noticing a striking side effect: significant, sustained weight loss.
Advert
In response, newer formulations and dosing strategies were approved specifically for people with obesity or those at high risk of weight-related conditions.
Today, and after the drugs caught on in celebrity and influencer circles for their weight management benefits, these medications are being used far more widely, not just by patients with diabetes, but by individuals seeking to manage weight, reduce health risks, or address long-standing metabolic issues. Doctors have also warned about potential side effects.
What’s drawing increasing attention, however, is that their impact may extend well beyond the scale. Emerging research suggests these drugs could influence a range of biological systems, from cardiovascular function to brain chemistry. As their use expands, scientists are beginning to uncover that these GLP-1 dugs could help the body in other ways.
According to in-depth research covered by The Washington Post, there is strong evidence suggesting that GLP-1s benefits for treating heart disease, liver disease, kidney disease and sleep apnoea.
Heart disease
There is evidence that GLP-1s help maintain cardiovascular health. Studies show they can significantly reduce the risk of heart attack, stroke, and death from heart disease, especially in people who are overweight or have Type 2 Diabetes.
Researchers believe this is partly due to weight loss, but also improvements in blood pressure, inflammation, and how the body processes sugar and fats.
The FDA approved semaglutide for cardiovascular disease in those who are overweight in March 2024.
Liver disease
The drugs show promise in treating liver disease.
A 2025 study published in the New England Journal of Medicine found that semaglutide improved outcomes in people with metabolic dysfunction-associated
steatohepatitis (MASH) and liver fibrosis.
MASH is a severe, progressive form of metabolic liver disease linked to obesity and broader cardiometabolic dysfunction, suggesting these drugs may help slow—or even reverse—serious liver damage.
Kidney disease
There’s growing evidence that GLP-1 medications can slow the progression of kidney disease, again particularly in people with Type 2 diabetes.
In January 2025, the FDA approved Ozempic to treat chronic kidney disease among those with Type 2 diabetes.
Sleep apnoea
Weight loss from these drugs can lead to fewer symptoms of Obstructive Sleep Apnea in people with obesity, a condition where breathing repeatedly stops during sleep.
Two major clinical trials found that tirzepatide significantly improved symptoms. Excess weight remains the leading risk factor for the condition
What are the theoretical benefits?
There are also theoretical benefits that are based on preclinical studies. There isn't enough evidence to say these drugs help in the following areas, but scientists and and doctors are keen to find out more.
One area includes fertility and social media has been flooded with reports of ‘Ozempic babies’, however there is limited data on the medications and fertility.
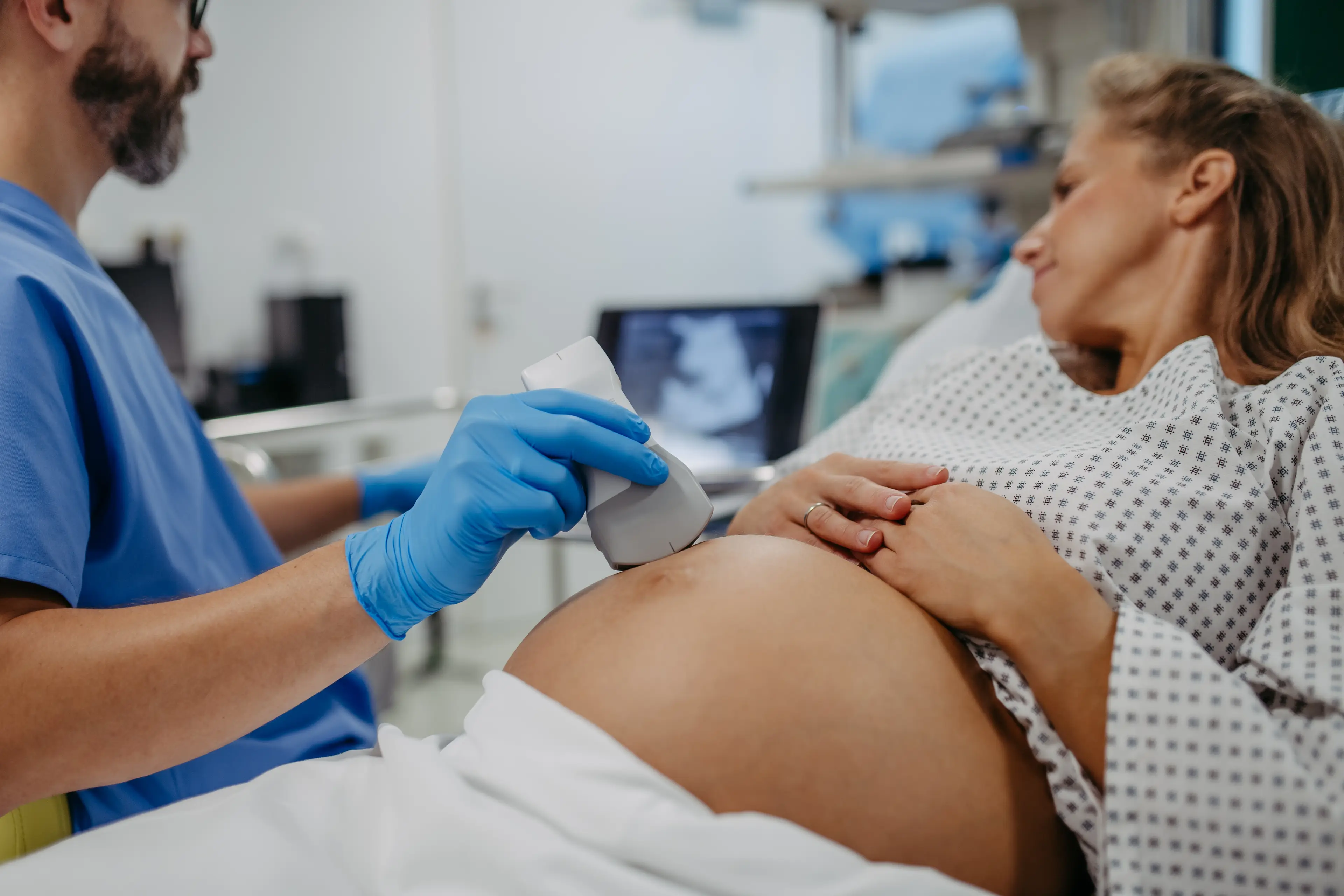
Some doctors theorise that surprise pregnancies are actually linked to the indirect benefits of treating diabetes and weight loss. Studies in the past have shown that getting pregnant can be more difficult for someone living with obesity.
Some evidence suggests these drugs reduce the risk of death and lowers the chance of serious complications in those who are infected with Covid-19.
Studies also point to potential benefits but also risks regarding cancer.
A study by researchers in the UK fond that patients on GLP-1 drugs had better control of their asthma symptoms, although the researchers did not find measurable improvements in lung function.
Elsewhere, some experts say GLP-1 drugs help to minimise physiological hunger and how the brain responds to food rewards, a process colloquially known as ‘food noise’.

