
Topics: Periods, Endometriosis, Women's Health, Health, Life, Real Life, True Life

Topics: Periods, Endometriosis, Women's Health, Health, Life, Real Life, True Life
A doctor has addressed an endometriosis sufferer's claim that the condition can affect the efficiency of birth control pills in preventing pain.
The assertion was shared by a woman named Natasha, who goes by the username @endometriosisandyap on Instagram.
Since joining the platform in November 2025, the online advocate - who suffers from Stage 4 endometriosis - has made it her aim to raise awareness of the often-overlooked realities of living with the chronic condition.
Endometriosis is a condition defined by cells that are similar to those that line the womb (or uterus), growing in other areas of the body. This often includes the ovaries, fallopian tubes and lining of the pelvis, but can also affect the bladder and bowel.
A hugely underfunded and under-researched area of women's health, it's a condition that can pose a devastating impact on the lives of its patients.
Advert
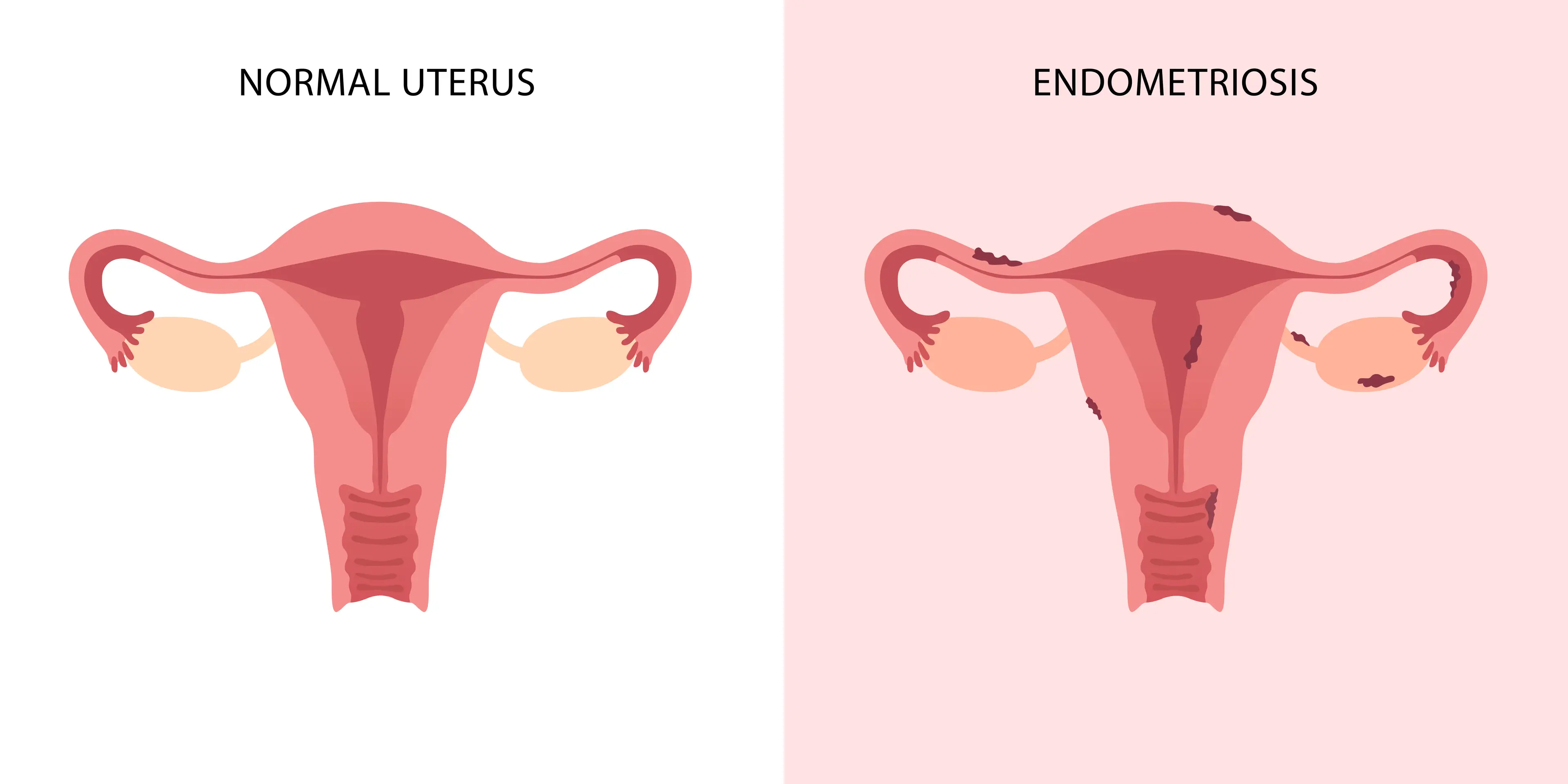
In the majority of recorded cases, sufferers battle severe period pain that prevents them from being able to carry out day-to-day activities, as well as heavy and often unmanageable bleeding.
Pain in the lower stomach and back is also common, along with pain when using the bathroom, pain during and after sex, and extreme fatigue.
The nature of endometriosis means the condition can also affect fertility and have a severe impact on the mood and mentality of its patients.
Women's health advocate Natasha has used her platform to share some of the most bizarre theories she's heard from certified doctors about her condition, as well as the tangible physical, mental and sociological impact that endometriosis has had on both her and fellow sufferers.
In a video shared earlier this month, Natasha honed in on the heavily-debated theory that endometriosis can cause the body to produce new levels of oestrogen, which she said can impact the efficiency of hormone medications, such as the contraceptive pill.
"Speaking of painful periods," she began. "We're often told that endometriosis is a hormonal disease, which is partially true.
"Endometriosis is certainly affected by hormones, especially oestrogen - but did you know that endometriosis also creates its own oestrogen?"
The content creator continued: "This is why birth control doesn't work for some of us, because birth control works via the body's natural hormone receptors, and endometriosis operates outside of those natural hormone receptors.
"So, you might be suppressing some of the oestrogen via your ovaries, but your endometriosis could be creating its own oestrogen."
According to the National Institute of Health, endometriosis is oestrogen-dependent, meaning, as Natasha explained, it is fuelled by fluctuating hormones.
It's oestrogen that promotes the growth of these painful lesions, and progesterone resistance that stops the body from being able to stop their growth.

As such, patients are often prescribed treatments aimed at reducing oestrogen levels during appointments with their GP, like birth control pills.
In more severe cases, surgery is also recommended. Natasha added, however, that the same pointlessness often applies in cases of a radical hysterectomy - 'where you remove everything including the ovaries'.
"You could take out the body's natural hormone factor, a.k.a. the ovaries," the social media star continued. "And endometriosis will be like, 'You think you did something there? Alright, bet', and create more oestrogen and grow more endometriosis, purely out of spite."
Natasha's claim has been backed by some experts at Endometriosis Surgical Specialists International, who agree that, while hormone medications can be effective in managing symptoms - especially period pain and flow - they don't eliminate the disease tissue that is actively producing its own oestrogen.

Responding to the viral video, however, Dr Susanna Unsworth - a women's health expert for the intimate wellness brand Intimina - explained that, while there's 'good evidence' to support the notion that endometriosis lesions can produce their own oestrogen on a local level, it may not apply across the board.
"Unlike normal endometrial tissue, endometriosis tissue has been shown to express aromatase, the enzyme needed to convert other hormones into oestrogen," she told Tyla.
"This means it can create a sort of self-sustaining, oestrogen-rich environment, where inflammation and oestrogen production reinforce each other and may help drive lesion growth and pain."
Issuing a warning against endometriosis patients ruling out hormone treatments like birth control pills altogether, however, Dr Unsworth continued: "If local oestrogen production were the whole story, we would not see so many patients responding well to treatments that suppress ovarian oestrogen, such as the combined contraceptive pill, progestogen-based treatments, or the hormonal coil.
"Equally, medications like GnRH analogues, which more completely switch off ovarian hormone production, can also be very effective for some people."
She went on to credit Natasha for raising awareness of the harsh realities of endometriosis, pointing out that her analysis of the issue 'may help explain why some cases are more persistent or treatment resistant'.
The doctor went on to point out, however, that hormone production is 'probably only one part of a much more complex condition'.
"Endometriosis is still fundamentally an oestrogen-dependent disease," Dr Unsworth continued. "But the source of that oestrogen and how the tissue responds to it appears to vary between individuals.
"This may also link to other factors we see in endometriosis, such as progesterone resistance and altered hormone receptor signalling."
Asked her final verdict, the medic emphasised: "The key takeaway is that the claim is broadly supported by research, but it needs nuance.

"It is not that endometriosis simply 'makes its own oestrogen' in all cases, but rather that some lesions may be able to generate oestrogen locally, which could contribute to ongoing symptoms in some patients."
She added, however, that overall, such debates emphasise the desperate need for further research on how women can realistically manage the life-altering realities of endometriosis.
"This is an evolving area of research and highlights why we still need a better understanding of the condition," Dr Unsworth concluded.