
Eight weeks into the national lockdown and life has changed beyond recognition for most of us.
But while the pandemic has forced many of us apart from our loved ones, every Thursday at 8pm we've all been united in a sea of applause as we take to our doorsteps to clap for our carers.
As the daughter of two NHS workers, I've seen first-hand how much this national display of gratitude means to those working on the front line. But, as wonderful is it is to praise the heroism of NHS staff, it's important to remember they're not martyrs, or superheroes. They're people, just like you and me.
Advert
Since the pandemic took hold, some 50 per cent of NHS employees have seen their mental health deteriorate, with younger workers reporting a 71 per cent decline - more prominent still in women.
Many frontline workers have been left scared to go to work as a result of PPE shortages, and, most heartbreakingly of all, a total of 181 have so far lost their lives while protecting the public from this invisible killer.
This is the story of five young women on the front line of the coronavirus crisis, as told to Tyla.
...............................................................................................................................................
Advert
"You'd be naive to think that some frontline healthcare workers won't leave this pandemic with PTSD"

Francesca Jackson Spence, 26 - A&E Doctor at Royal London Hospital
As a junior doctor, Frankie was rotating between different departments when the coronavirus pandemic struck, and was abruptly taken off her placement as a GP to go and work in A&E.
Advert
"I was anxious, because I was given two days' notice and I've never done emergency medicine before," she tells Tyla. "But I was also excited to be at the front of it, as I don't think there will be anything like this again in my medical career".
One thing that was abundantly clear as she arrived was the lack of non Covid-19 patients.
"This was actually quite concerning; [it seems] a lot of people having heart attacks, strokes and chest infections were staying at home because they were afraid to come to hospital," she says.
The coronavirus patients she sees are typically seven to 10 days into their illness, and tend to be showing chest tightness, difficulty breathing and low oxygen levels, while many also exhibit flu-like symptoms.
Advert
When they arrive in A&E, it's Frankie's job to try and treat them with varying levels of oxygen. But she's also tasked with making them feel comfortable when they're scared and, most often, alone.
"Now is a particularly horrible time because people aren't allowed to have family members with them [on the ward]," she says.
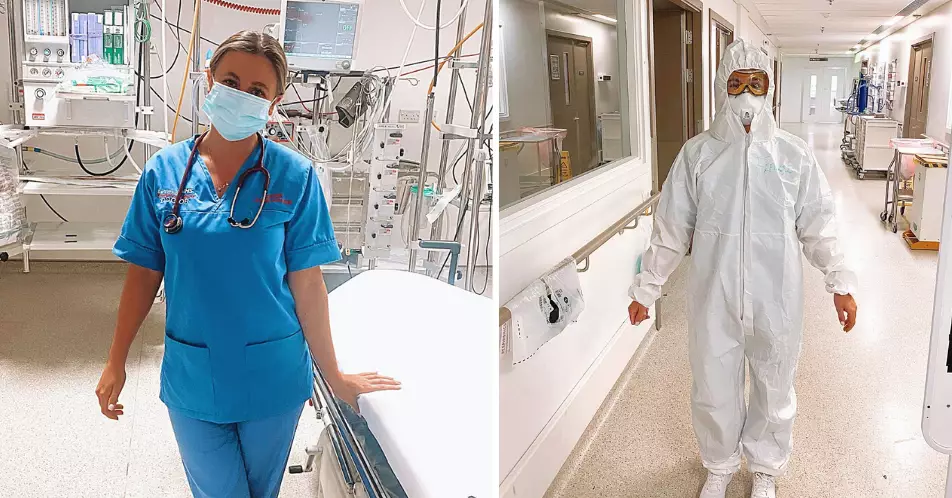
"They're rushing into this busy emergency department on their own with bright lights, their oxygen masks are often uncomfortable, and then they're greeted by doctors and nurses dressed head-to-toe in PPE, so they can't see us smile. It must be so daunting."
Advert
Despite the necessary limitations of PPE, Frankie says the pandemic has actually encouraged her to spend more time getting to know the people she's treating.
For example, recently "there was this old man, and I could tell he was really afraid," she says. "So I just sat with him for an hour after my shift and let him tell me about how he met his wife, his kids and grandchildren, and how he's liked having them all at home during the lockdown.
"There's a chance he won't survive Covid-19 - I might be one of the last people he sees - and, more importantly, that hour probably made him feel less anxious and alone."
Dealing with cases like this on a regular basis is heartbreaking, Frankie admits. "I think we'd be naive to think that some frontline healthcare workers won't leave this pandemic with PTSD."
She adds: "Occasionally, there are times when being a doctor can feel like a thankless job. You'll think you've gone the extra mile and done something particularly well, but when patients are in pain and families are stressed, they may think it's the norm.
"There is a lot of sacrifice in medicine. But the reward is mainly personal: it's feeling like you've done a human job".
...............................................................................................................................................
"You and your loved ones do not want to be in the position that our patients are in"

Georgia, 24 - Respiratory Physiotherapist at Weston General Hospital, Weston-super-mare
Georgia, who has been in her current job for three years, believes physiotherapists have not always received the same recognition as other professionals working on the front line.
"We are renowned for treating injuries, but not many people realise that in hospitals there are respiratory physios who treat chests too," she tells Tyla. "I've had many people who've been shocked to find out that I work on intensive care, and even then they think that [all we do is] stretches."
Despite these misconceptions, physiotherapy has proven a vital lifeline for Covid-19 patients during every stage of their treatment.
On the intensive care unit (ICU), Georgia conducts breathing assessments on coronavirus patients, as well as treatments for those on ventilators, to help strengthen their respiratory systems and prevent their lungs from collapsing.
She also provides aftercare for those who make it off the ventilators - for many it's an "extremely long" road to recovery - and end-of-life care for those who don't.
In those cases, her job is to help dying patients into more supportive, comfortable positions, and teach them relaxed breathing control, which can manage their breathlessness and anxiety.
Georgia admits that, after building a rapport on the ward, watching a patient pass away can have a heavy emotional toll - but as tough as it can be at times, "knowing that we can help them at each part of their life makes our job worthwhile."
Of course, amid the sad stories, there are happy endings too; one patient Georgia remembers fondly is a 78-year-old man, whose chest she spent two weeks treating on an ICU ventilator. She later provided rehabilitation throughout the rest of his stay, to help build his muscle strength.
"After a huge fight from him, he was successfully taken off the ventilator and we were eventually able to discharge him from intensive care onto a ward," she says. "He is now Covid negative. We were extremely excited to be clapping him when he left hospital."
Reflecting on the last two months and her hopes for the future, Georgia adds: "I just beg that people don't get frustrated or slack with social distancing as the weeks go on. We're the ones who are seeing daily how detrimental this virus is and how it does not discriminate, no matter what age you are or your medical history.
"So, please, take our word for it that you or a loved one does not want to be in the position that our patients are in."
...............................................................................................................................................
"I've made the decision to move away from my family for however long this may be"

Rani Bathia, 30 - GP Registrar at Parkbury House Surgery, St Albans
Like many front line workers across the country, final-year trainee GP Rani has had to adapt to some major changes since the coronavirus pandemic unfolded.
Firstly, her GP training has been cancelled to ensure "all energy is saved for patients". Plus, most appointments at her surgery now take the form of video consultations and phone calls, and patients are "risk stratified" - meaning they're only seen in person at a different site if absolutely necessary, and if they are showing primarily non Covid-related symptoms.
"One positive is that this has been a huge catalyst for technology to help us see patients day-to-day," she says.
But despite the stringency of these new safety measures, the unavoidable risks attached to her job have still trickled into her personal life.
"I've made the decision to move away from my family for however long this may be," she tells Tyla. "My biggest fear was giving [the virus] to them. Obviously this bears psychological burdens, it bears financial burdens, but that was not a risk I was wiling to take.
"The thought of being unknowingly asymptomatic and passing something onto them... I wouldn't be able to live with that."
As well as the knock-on affect the virus is having on her own life, Rani is also seeing first hand just how much it is affecting her patients.
Some appointments and scans have been cancelled due to the pressure on the healthcare system, and even if they do go ahead, patients are fearful to attend - a phenomenon she's dubbed "coronaphobia".

And while the majority of people with coronavirus symptoms are calling 111 rather than the surgery, Rani explains: "It's not just coronavirus we're dealing with, it's the whole impact that coronavirus has had on society".
"The amount of mental health [patients] we're seeing now has significantly increased," she says. "Firstly, that's down to fear of catching the virus.
"But it could also be that they have longstanding mental health problems, or things like OCD or anxiety, which have obviously been heightened at the moment, or even new diagnoses of significant mental health issues, like psychosis. We underestimate the impact of changes in people's lives."
And what about her? "GPs have similar emotions to others," she concedes. "And psychologically, it does have a huge impact. You come to work and you spend your time focused on others, and subconsciously you take a degree of that onto yourself.
"The medical profession take on a lot of risk and we have people's health in our hands. It's really nice to see so much support of the NHS, but you hope that people continue to maintain the level of respect afterwards".
...............................................................................................................................................
"I just kept thinking: 'What if this was my nana or my granddad?'"

Rosie NC, 25 - Bank Healthcare Assistant across Barts Health NHS Trust
Rosie has been a bank healthcare support worker since October 2018, but having spent that time assisting in a sexual health clinic, her first shift in ICU was something of a baptism of fire.
"My first Covid-19 ward experience was my first ever 12-and-a-half-hour shift, and it was a lot. Hospital ward culture is very different anyway, and to have the pandemic atmosphere was very intense," she recalls.
"I remember I introduced myself to a nurse who was in my bay, which was a section of the ward I'd been assigned to - at this point, we were all in PPE, meaning our faces were completely covered.
"I kind of muffled through the mask, 'Hi, I'm Rosie, how are you today?' And the nurse just replied: 'scared' and then carried on doing his job.".
As a healthcare assistant, Rosie's duties range from changing sheets to taking lunch orders to observations, taking blood pressure, oxygen saturation and pulse rates, depending on which ward she's on.
While she spent the majority of her first ICU shift running around and getting nurses the drugs and equipment they needed, one moment in particular has stuck with her.
"There was one very young asthmatic patient. I took him to the toilet and we had this bizarre moment where we were just chatting about uni and stuff - having a normal conversation," she recalls.
"Then, all of a sudden he was just like 'I need oxygen,' and we crashed back down to earth. He was actually younger than me, which was strange. It does hit home".
Like many frontline workers, she has shifts where she feels "invigorated," and "part of the fight" - just the other day, she saw a 92-year-old granddad leave ICU.
"But there have been a few much harder days," she says. "There was one shift where I was the only healthcare assistant in a ward of 30 patients, and there was four or five poor nurses, and I just remember they all looked drained... morale was low."
"When I got home, I wasn't hungry. I was really tired but I couldn't sleep, and I just had to pick up the phone to my mum and cry.
"It was just seeing the horrible and distressing impact of what happens when a ward is so short-staffed that it's almost an impossible task to maintain a high level of care that people deserve.
"It was nobody's fault, but it felt really distressing. I just kept thinking, 'What if this was my nana or grandad?' I was heartbroken".
As a 'bank' NHS worker, Rosie is under no obligation to work shifts, but she does so anyway.
"Some of my friends [say], 'I don't understand why you're doing this," she says. "On the whole there is a fear from my loved ones, but I know I'll be fine because I have the luxury of being able to pull back if it's getting too much.
"I worry more for my friends who have to do this [job] whatever the weather. I really hope everyone manages to come out of this unscathed".
...............................................................................................................................................
"We are concerned about the low numbers of children coming in"

Sophie McGowan, 20 - Paediatric nursing student, John Radcliffe Hospital, Oxford
Sophie was nearing the end of her three-year nursing degree when she was suddenly called to work.
"I was about to start my final 12-week placement on one of the children's wards at the John Radcliffe Hospital and then all of a sudden I was sent to work on a children's Covid-19 ward," she says.
"It was very nerve-racking, we all sort of had a bit of a panic... a bit of an 'oh no' moment. Jumping into it all was very daunting, but I had done three years, and just had to tell myself I was fine".
The area Sophie is working in was once a general respiratory ward at the hospital, but has been transformed into a paediatric Covid-19 ward for the duration of the crisis.
While it's common knowledge that children's symptoms are generally less severe, she says they've been "taken aback" at the small number of children being admitted, and relieved that, on the whole, they've barely needed more than a few days of care.
That said, there are concerns that the lack of admissions on non-Covid wards alike represents a wider issue.
"We are worried," Sophie admits. "Parents aren't taking their kids to be vaccinated out of fear, and we are concerned about the low numbers of children coming in to A&E."
This anxiety is clear among those parents who do come in, too - especially when they find out their children are being put on a Covid-19 ward while they're being tested, or worse still that they have the virus.
"Parental anxiety is probably one of the biggest things we've had to deal with at the moment," she says. "I'm used to this to some extent, because every time a child comes into hospital parents are anxious, but it's the unknown at the moment that's adding to it."
As for the children? Most of them are too young to understand, she says.
But when she does have to explain the virus to those she's treating, she's been struck by their positivity and resolve.
"One 11-year-old girl always said: 'today's not been great, but tomorrow's another day,'" she recalls.
"Children are a lot more optimistic, and I've not met a lot of children who focus in on the negative. It's nice to look at that sort of mentality and remind yourself it's not forever.
"It would be good to pick that up from children. They're doing it right!"
If you want to help NHS staff you can donate to NHS Charities Together here.
Topics: Life News, News, Real, Coronavirus, NHS, Life News, News, Real, Coronavirus, NHS