
Welcoming a new baby into the world should be a happy occasion, but giving birth can lead to hugely serious complications for many women.
While conditions such as post-natal depression are well-known, fewer are aware of Postpartum Psychosis, the rare but incredibly serious mental health condition that the NHS class as a medical emergency - which only affects to one in every 1000 women who give birth.
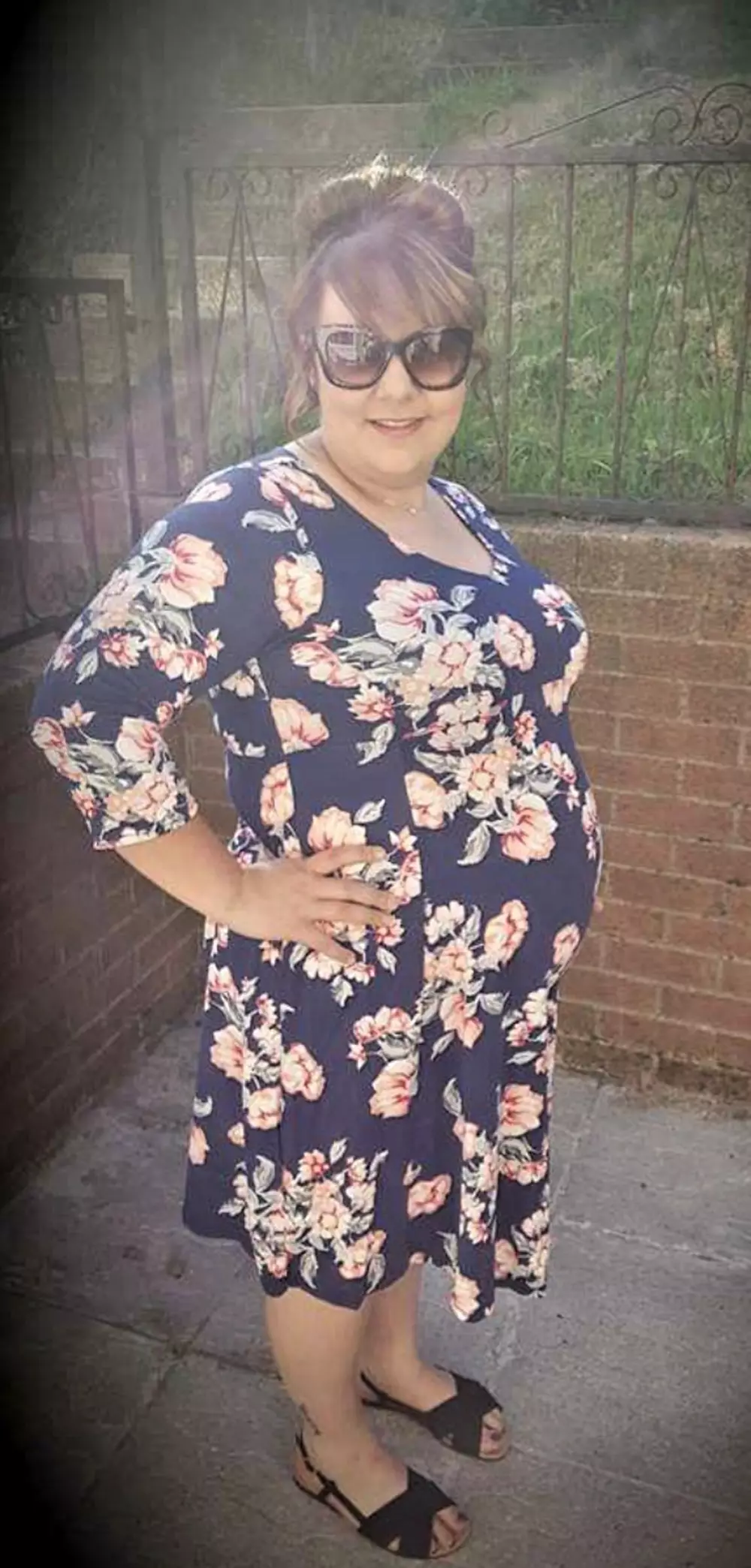
Midwife Danielle Thomas, from Newport in South Wales, was delighted when she discovered she was expecting a baby.

Alongside her husband Darren, Danielle made a birthing plan once she passed the 12 week milestone, which would see her having her daughter, April, now three, in her nearby hospital's birthing centre.
Advert
However, when she passed her due date by two weeks, Danielle's initial plan was crumbled and she found herself having to have a C-section on a labour ward after being induced.
The birth was traumatic and lead to subsequent haemorrhaging, which is what is likely to have triggered her Postpartum Psychosis.
"I was exhausted, in pain and also the baby's head was in such a position I knew it wasn't possible for her to be born without intervention, so we agreed to the C-section," Danielle explained.
"I was nervous and anxious and in floods of tears. I've looked after lots of patients about to have this procedure, but this time it was happening to me."
Advert
While she was happy when April had been delivered, Danielle quickly felt the feeling of being overwhelmed with her baby.
"I felt battered, in pain and as if I had been hit by a bus," she said. Everyone was congratulating us and telling me I'd be fine in a couple of days, but I didn't feel fine."
Danielle didn't initially recognise the symptoms of Postpartum Psychosis, but was in the thick of the condition by the time she arrived home.
She had irrational fears that her dog, Lyra - who is usually calm and placid - could attack baby April.
Advert
She was also fixated on the pain of the birth, which she talked about with visitors and relived at night when she couldn't sleep.

"By then I wasn't eating or sleeping," she said. "I'd be up doing the laundry at 3am and I was starting to resent Darren.
"I'd feel jealous that he could finish his meals whereas I'd have to jump up and feed the baby.
Advert
"I started rowing with him and, eventually, because I didn't want us to be arguing around April, I told him to pack his bags and leave."
It was when Danielle tried to physically force Darren out the house that he sought help from both their mothers, who then tried to persuade Danielle to see a doctor.
"They were telling me I needed to see a doctor and I was shouting at them.
"I would never normally speak to my mum or my mother-in-law that way, so it was obvious to them something serious was wrong with me, but I couldn't see it.

"I shouted at them for ganging up on me and said it was just post-natal depression, nothing more.
Advert
"They called an out-of-hours GP and I told him it was Darren who was struggling, not me. I rambled on and on. It was like I had verbal diarrhoea.
"The GP did not think I was a risk to April and so did not section me but told me I was to go to the assessment unit at the hospital.
"I didn't want to go, so my mum cleverly tricked me by pretending we were just going to take the baby for a walk around the place where I'd had my scans and ante-natal care, which I thought was a great idea."
After assessments, which Danielle failed, the new mum became increasingly distressed - which saw her grip on reality loosen. When she was sectioned after the assessment and taken directly to the hospital's secure acute mental health ward, she thought she was being shown around because she had just landed a new job there.
"I became more and more confused," she said. "I forgot I even had a child and was running around talking to everyone and trying to make connections that didn't exist between them and my life outside the ward."
Danielle also spent most of her first few days on the ward planning her escape.

"I felt like I was somehow in one of those Escape Room games and that if I could only put the clues together, I could work out how to get out," she said.
"That first day I was shouting and verbally aggressive. I wouldn't take my anti-psychotic medication, because I thought they were all trying to kill me.
"I remember lifting up my shirt and looking at my Caesarean scar.
"Some part of my mind was telling me I had a baby, but I didn't know where the baby was. Of course, she was at home with my family."
Eventually, it took Darren falling to his knees and pleading with Danielle to take her medication for her to relent.
And, for the first time since April's birth, she went to bed and slept - for an entire night and the whole of the following day.
This time, when she woke up, although she did not know where she was or why she was there, she at least felt like herself again and knew who she was - also remembering that she had given birth to a baby girl.
After spending six nights on the hospital's psychiatric ward, she was then transferred to a mother and baby unit in Winchester, Hampshire, where April joined her for another 10 nights.
With additional support, medication and therapy, Danielle slowly recovered from her psychotic breakdown - something doctors believe to be caused by a chemical imbalance in the brain.

She continued to experience severe post-natal depression for eight months, but Danielle said her sanity was restored and she has not looked back.
Happily engaged to Darren and with the pair now trying for another baby, Danielle now works as a volunteer for the Action on Postpartum Psychosis charity, which supports other new mums that may experience this harrowing condition.
"It isn't easy to talk about what happened and, for a long time, I was scared to tell anyone in case they judged me or thought I was crazy," she said.
"There is still a stigma around anything to do with mental health, so I want to use my platform as a midwife to help others by saying this is out there and it can happen to anyone."
Featured Image Credit: PATopics: Children, Life News, Mum, Life, Babies, Birth, Motherhood, Mother