
The National Institute for Health and Care Excellence (NICE) has revealed a proposal to induce labour in Black expectant mothers at 39 weeks to reduce risks and inequalities in birthing outcomes.
According to the NHS website, an induced labour is one that is started artificially and every year one in five labours are induced in the UK.
An induced labour is usually brought on if the baby is overdue - if the pregnancy lasts longer than 42 weeks - or If the mother has health conditions such as high blood pressure.
Advert
The guidance from NICE is still in its draft stage and recommends that healthcare professionals should consider offering induced labour to Black, Asian and ethnic minority women a couple of weeks before their pregnancy reaches full term.
This comes after findings that women from these backgrounds are at a higher risk of adverse events in pregnancy that lasts more than full term.
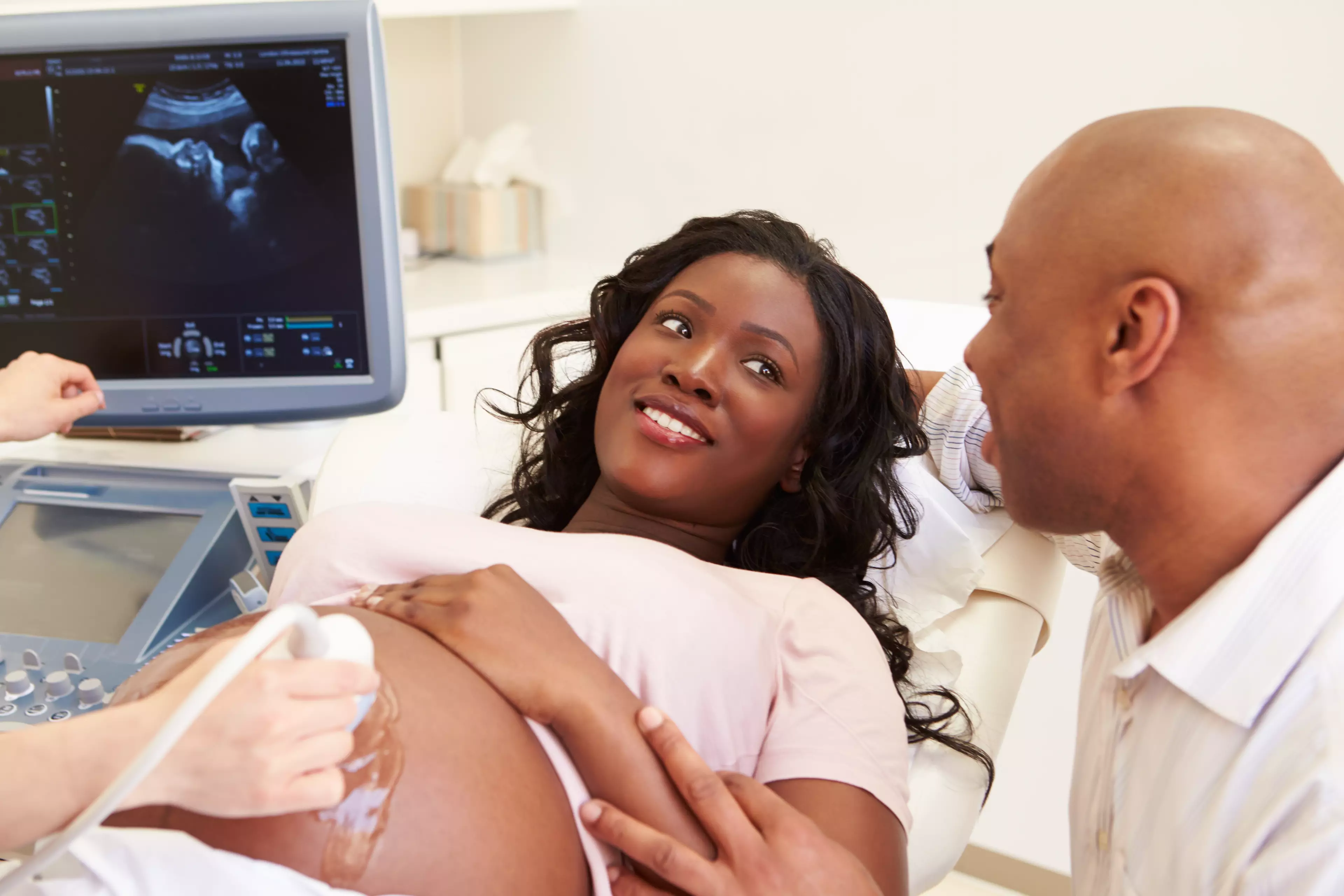
Research has found that Black women are more prone to conditions such as high blood pressure and diabetes which can cause complications during labour.
Advert
In 2020, a damning report published by Parliament found that Black mothers are five times more likely to die than white mothers during or after pregnancy and giving birth.
The report was published in November 2020 following the Black Lives Matter protests earlier in that year and the death of popular YouTuber Nicole Thea when she was eight months pregnant in July. The report's conclusion reads: "The NHS acknowledge and regret this disparity but have no target to end it."
There are also concerns that racist stereotypes and discrimination, such as those claiming that Black women have a higher pain threshold or that Black skin is less sensitive, may also play a part in concerns such as back pain and other symptoms being ignored by healthcare professionals.
Advert
Twitter users expressed outrage following news of the proposal using the hashtag #NotSoNice. "The problem isn't being Black & giving birth," wrote one person. "The problem is the systemic racism in the maternity system."
Another woman spoke about her own experience of being induced. "I was induced just over 37 weeks with my first, was left without pain relief, food or water and ended up vomiting on myself as I was told I could not move in order for them to monitor my baby. It resulted in a cascade of interventions. This is not a solution."

Similarly, a mother shared: "I gave birth at 41+5 days to my youngest son and received woefully inadequate care, putting me and my son at risk. Being induced at 39 weeks wouldn't have prevented the structural issues I faced! #NotSoNice this is even seen as a solution."
Advert
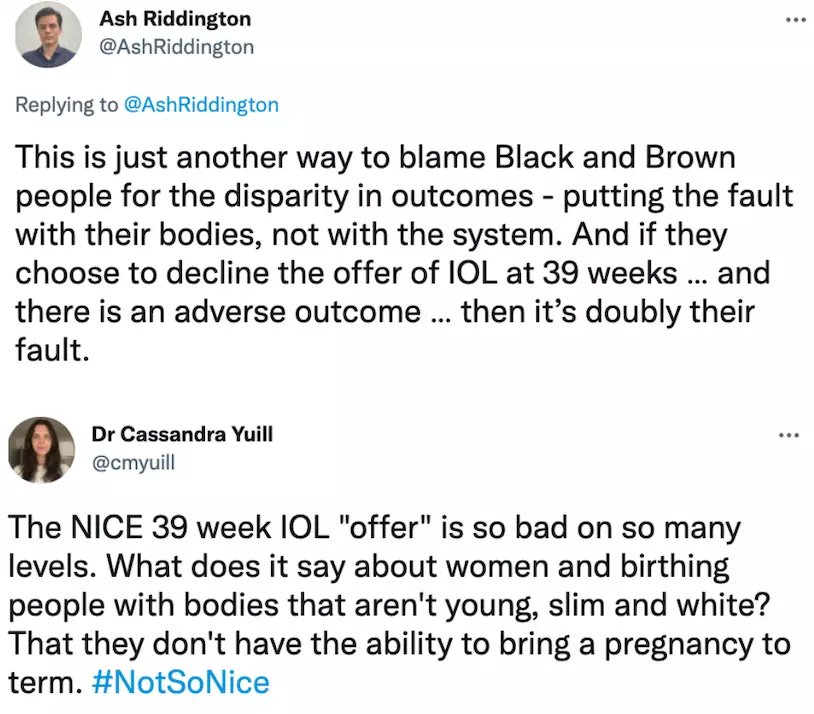
Midwife Ash Riddington tweeted he was 'absolutely disgusted' by the new NICE guidelines and posed the question what happens to Black and brown people's pregnancies at 39 weeks that doesn't happen for white women. "This is just another way to blame Black and brown people for the disparity in outcomes - putting the fault with their bodies, not with the system. And if they choose to decline the offer of IOL (Induction of Labour) at 29 weeks.... And there is an adverse outcome... then it's doubly their fault."
Dr Cassandra Yuill said: "The NICE 39 week IOL 'offer' is so bad on so many levels. What does it say about women and birthing people with bodies that aren't young, slim and white? That they don't have the ability to bring a pregnancy to term. #NotSoNice."
A NICE spokesperson told Tyla: "The recommendations in this draft guideline are subject to change based on the comments we have received during the consultation period. We welcome feedback on draft recommendations and will consider all comments we receive during consultation.

"The draft recommends healthcare professionals consider offering induced labour to this group of women from 39 weeks. However, healthcare professionals must discuss the risks and benefits of induced labour with the woman and take her preferences into account. They should respect and support her decision if she chooses not to have labour induced.
Advert
"The draft guideline also calls for more research into understanding the optimal timing of induction of labour in women from Black, Asian and minority ethnic backgrounds, as better evidence is needed in this area.
"It's clear there are still significant health inequalities in maternity outcomes which need to be addressed, and we hope the final recommendations will go some way towards doing that."
The consultation period ended on 6th July 2021. The final guideline is expected to be published in October 2021.
Featured Image Credit: Shutterstock